Genetic Testing: A Right Not to Know
The other day I picked up an article from The Wall Street Journal that caught my attention for many reasons. I have always personally struggled with the concept of genetic testing. On the one hand, I think it is an amazing feat. Pre-implantation genetic diagnosis would grant me the ability to check and make sure my kids are born healthy. Personally, that is something that greatly tempts me, because I would never want my child to have to suffer through anything that I could have potentially prevented. However, on the other hand, I am a strong believer in “everything happens for a reason.” My mother has instilled in me the belief that, “in life, you will only be granted what you can handle, so there is no need to worry.” With these moral principles ingrained in my being since the beginning, I face a personal ethical dilemma. Thankfully, I do not have to make these kinds of decisions in my life just yet. However, I found this article very interesting and a step in the right direction for the future of genetic testing.
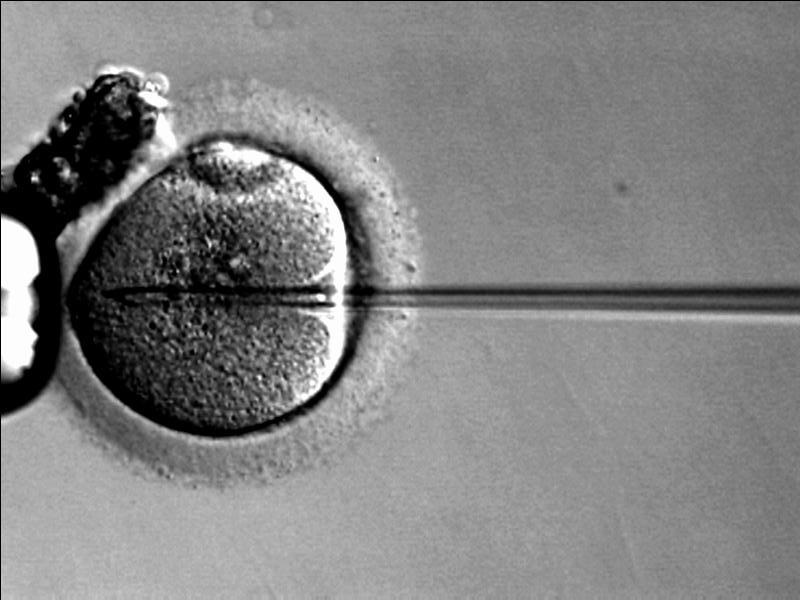
One of the largest ethical issues regarding genetic testing is the patient’s right to know, or for that matter, their right to refrain from knowing. This particular article spoke of a patient who came in for a pre-implantation genetic diagnosis for a particular gene mutation that causes early onset Alzheimer’s. This gene mutation ran in the patient’s mother’s family, so the patient wanted to make sure the embryo that would be implanted in her did not code for that gene mutation. This would ensure the soon-to-be mother that her child would not be born with the gene mutation. What was unique about this situation is that although they tested the embryo for the gene, they never tested the mother’s DNA, nor disclosed to her the number of embryos that had, in fact, coded for that gene mutation. The doctor in this case respected the patient’s decision to not know. This story in many ways illuminates a current ethical battle genetic testing faces.
Should patients have the right to refrain from knowing? What if early prevention could save a patient’s life?
A quote from the above article reads, “Last year, the American College of Medical Genetics recommended that incidental findings of 56 genes representing several conditions must be disclosed to patients.” Clearly, this was met with resistance due to the fact that many patients do not want to know because knowing can cause extreme stress and anxiety. Yet, on the other hand, some of these genes code for conditions that, if treated early, can be prevented or at least symptoms could be lessened. This creates a difficult ethical dilemma for doctors who strive daily to save lives.
From my perspective, I think that although doctors may feel obligated to tell their patients, it comes down to whether or not the patient wants to know. Doctors must respect their patients wishes, because ultimately, it’s not their life, it’s the patients. Doctors can fulfill their moral obligation by letting patients know that they have results from genetic testing that may be beneficial to know, but the patient must request that they want to know more for the doctor to disclose further information. I think that in the situation above, the doctors were ethically correct in how they respected by the patients request not to know, while also taking measures to ensure that her children would be born healthy.